|
Outsourcing DME billing helps in numerous ways. Yes we understand that you have your own billing department. But it’s true and well said that when you get a service outsourced the work is done by sheer professionals who are not just confined to the task they are given. These professionals are so accurate and experienced with their work that they even know how to take more out of it.
DME (durable medical equipment) outsourcing can make your billing department focus on the patients bills solely without being distracted to other types of billing anyway. Outsourcing DME billing will help you. You don’t have to hire for anything which is remotely related to DME billing. Outsourcing can help do it all for you. Outsourcing billing will also help your company grow, rise and think of more effective business strategies instead of just focus on billing and collecting equipments. No doubt billing is foremost feature when in a business but doing it efficiently is the principal key to zero fraud. Let your company focus on giving best services for patients. Futuristic Gigatech, one of the most frequently asked billing company is there to outsource your billing work more efficiently. Rather the Futuristic Gigatech, healthcare analytics company will not only outsource the DME, (durable medical billing) but will also focus on rehabilitation, mobility, powered ability, aids, respiratory services and many more. So make the best of outsourcing and focus on the expansion and best facilities for your patients.
1 Comment
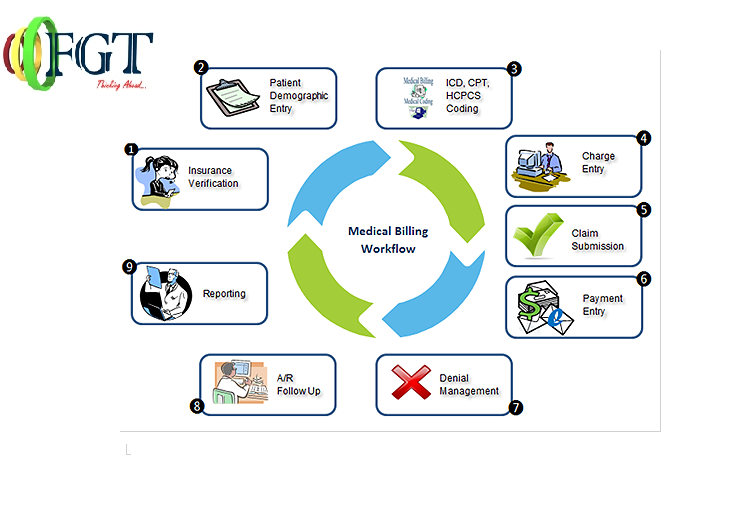
Medical billing might seem large and complicated than medical coding but it’s actually a process that’s comprised of eight simple steps.
The billing process of medical billing is simply stated as the process of communication between the medical provider and the insurance company. This is known as the billing cycle. The medical billing cycle can take in upwards of days to months to complete, and at times take several communications before resolution is reached. Following steps of process are below: 1. Register Patient: When a patient calls to set up an appointment with a healthcare provider, they effectively preregister for their doctor’s visit. If the patient has seen the provider before, their information is on file with the provider, and the patient need only explain the reason for their visit. If the patient is new, that person must provide personal and insurance information to the provider to ensure that that they are eligible to receive services from the provider. 2. Financial Responsibility: Once the biller has the pertinent info from the patient, that biller can then determine which services are covered under the patient’s insurance plan. If the patient’s insurance does not cover the procedure or service to be rendered, the biller must make the patient aware that they will cover the entirety of the bill. 3. Patient check-in & check- out: When the patient arrives, they will be asked to complete some forms or confirm the information the doctor has on file. The patient will also be required to provide some sort of official identification, like a driver’s license or passport, in addition to a valid insurance card. Once the patient checks out, the medical report from that patient’s visit is sent to the medical coder, who abstracts and translates the information in the report into accurate, useable medical code. This report, which also includes demographic information on the patient and information about the patient’s medical history, is called the “super bill.” 4. Prepare claims: The medical biller takes the super bill from the medical coder and puts it either into a paper claim form, or into the proper practice management or billing software. Once the claim is approved the medical provider is reimbursed based on a pre-negotiated percentage. Any rejected claims are sent back in the form of Explanation of Benefits or Electronic Remittance Advice. 5. Transmit claims: Billers may still use manual claims, but this practice has significant drawbacks. Billing electronically saves time, effort, and money, and significantly reduces human or administrative error in the billing process. Instead of having to format each claim specifically, a biller can simply send the relevant information to a clearinghouse, which will then handle the burden of reformatting those ten different claims. 6. Adjudication of Monitor : Once a claim reaches a payer, it undergoes a process called adjudication. In adjudication, a payer evaluates a medical claim and decides whether the claim is valid/compliant and, if so, how much of the claim the payer will reimburse the provider for. It’s at this stage that a claim may be accepted, denied, or rejected. Effectively, a claims appeal is the process by which a provider attempts to secure the proper reimbursement for their services. This can be a long and arduous process, which is why it’s imperative that billers create accurate, “clean” claims on the first go. 7. Patient Statement : Once the biller has received the report from the payer, it’s time to make the statement for the patient. Once the payer has agreed to pay the provider for a portion of the services on the claim, the remaining amount is passed to the patient. 8. Follow up patient statement & collections : The final phase of the billing process is ensuring those bills get, well, paid. Each provider has it’s own ways, set of guidelines, timelines. So you’ll have to refer to the provider’s billing standards before engaging in these activities. Futuristic gigatech undertake services both in standard bill review and clinical bill review. With our blended knowledge in medical, bill review knowledge, and technology we fill the gap between utilization review and bill review. It’s the best medical billing company in Bangalore. For more detail visit-: http://futuristicgigatech.com/ Medical billing & Medical coding can be a demanding and challenging task for small medical practices.
Most of the medical companies and hospitals are adopting the facility of medical billing and medical coding. Medical coding and billing services are used for both administrative and clinical purposes, every department within a health care organization benefits from the advantages of these medical processes. Several benefits which a firm can get by adopting these medical services are: Higher and faster collection rate: The companies having the expertise in this area will provide higher collection rate than other clinic groups and hospitals who attempt collections on their own. The speed with which the money gets collected can affect the overall operations of the medical practice. Faster claim processing is conducted by the companies providing medical billing and medical coding services which ensures healthier cash flow. Access to expertise services: The complexities of medical billing and medical coding are growing day by day making it mandatory to have a standardized way of using medical codes to perform regular internal reporting. By hiring or outsourcing these services a firm gets the access to the expertise services. These tasks are performed by a specially trained professional of the outsourcing partners. But by using the services of Futuristic Giga Tech Pvt. Ltd which is one of the best companies providing services in medical billing and medical coding in Bangalore, medical firms will not have to carry added overhead year around in hiring and training specialized staffs. It's time for you to hire our Medical Billing Services. We ensure to deliver the best services for your healthcare organizations! Medical billing and coding are two closely related aspects of the modern health care industry. Both practices are involved in the immensely important reimbursement cycle, which ensures that health care providers are paid for the services they perform. When a patient has any medical exam or procedure, the medical office will work with the patient and the patient's insurance company for claims. The biller will submit and follow up on any claims in order to receive payment for services rendered by the health care provider. This usually involves learning many codes, each one representing a symptom, medications and diagnoses, in order to process the claim properly. Medical billing and coding workers are the health care professionals in charge of processing patient data such as treatment records and related insurance information. Medical insurance billers and coders are tasked with coding a patient's diagnosis along with a request for payments from the patient's insurance company.
Medical Coding: Medical coding, at it’s most basic, is a little like translation. It’s the coder’s job to take something that’s written one way. For example -: A patient walks into a doctor’s office with a hacking cough, high production of mucus or sputum, and a fever. A nurse asks the patient their symptoms and performs some initial tests, and then the doctor examines the patient and diagnoses bronchitis. The doctor then prescribes medication to the patient. Every part of this visit is recorded by the doctor or someone in the healthcare provider’s office. It’s the medical coder’s job to translate every bit of relevant information in that patient’s visit into numeric and alphanumeric codes, which can then be used in the billing process. The coding process ends when the medical coder enters the appropriate codes into a form or software program. Once the report is coded, it’s passed on to the medical biller. Medical Billing: On one level, medical billing is as simple as it sounds: medical billers take the information from the medical coder and make a bill for the insurance company, called a claim. Of course, as with everything related to the health care system, this process isn’t as simple as it seems. Let’s take an example-: Our same patient has a cough, a fever, and is producing lots of mucus. This patient calls the doctor and schedules an appointment. It’s here that the medical billing process begins. The medical biller takes the codes, which show what kind of visit this is, what symptoms the patient shows, what the doctor’s diagnosis is, and what the doctor prescribes, and creates a claim out of these using a form or a type of software. The biller then sends this claim to the insurance company, which evaluates and returns it. The biller then evaluates this returned claim and figures out how much of the bill the patient owes, after the insurance is taken out. The biller has a number of other responsibilities, but for now you should simply know that the biller is in charge of making sure the healthcare provider is properly reimbursed for their services. At Futuristic Giga Tech Pvt Ltd our state-of-art facility and services offers cost-effective and timely patient scheduling services. Our teams verify and validate the documents, split them into batches and review them for completeness, quality and readability. For more detail visit-: http://www.futuristicgigatech.com/ Futuristic Gigatech is one of the best health care service provider in Bangalore. We are able to achieve this just because of our working scenario and the process we follow to satisfy our client. Our clients are our first mandatory.
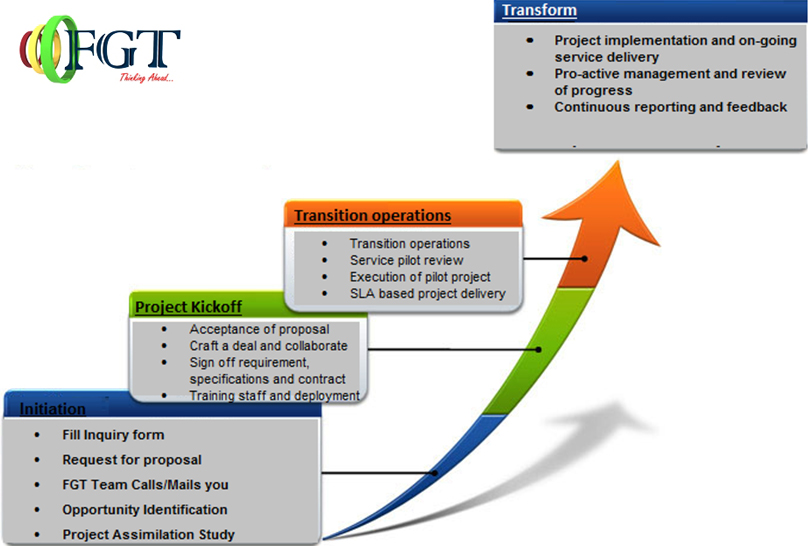
Futuristic Gigatech provides end-to-end medical billing services or a menu of services you pick and choose. It can be an individual practice, group practice, ASC or any hospital we ensure that you’ll receive the same Systematic attention to detail, superior customer care and best yet, guaranteed results. Our best services helps you to focus on your business and increase the productivity of the company by avoiding some repetitive and un-wanted task that lead to degrade your overall business performance. We follows the standard work flow procedure from initiation to transformation. Futuristic Gigatech have developed own proprietary state of the art Workflow Management tools. We have our own in-house dedicated software development team which has the following features. · End to end workflow management solution developed by our in-house dedicated Software. · Engineering Process Department. A medical practitioner comes across several challenges wherein; delivering the best patient care at an affordable rate, tracking Patient records and maintaining accessible patient history are essential elements of Patient care. But managing tons of paper and data undoubtedly gets them down. And this is where our role comes into play as we create a comprehensive Patient Record Management Platform. To overcome the increased challenges created by rising customer orientation, mounting routine work and unpredictable staffing needs, Futuristic Giga Tech Pvt Ltd- the best health care service provider in Bangalore is successfully serving in the healthcare sector since last few years. The higher aim here is to serve the nation and the health care organizations through the globe. In the last few years, the Healthcare industry across the globe has evolved and so have their processes. A larger number of countries are moving closer towards more comprehensive Healthcare for their citizens. Regardless of where the Provider / Physicians are located across the globe, managing patient data is becoming progressively more and more significant. The trick is to build efficient processes while keeping administrative costs down. Manage repeatable, benchmarked processes with the correct use of technology; get the advantage of Revenue Cycle Management (RCM). The present time demands one to focus on the core activity of offering medical services to patients while our specialist team takes care of the administrative & technology functions like Contracts Management, Electronic Medical Record Management, Eligibility Verification, Patient Management Software, Patient Scheduling, Claims Administration, etc. We support and maintain the quality of patient care giving you the added edge you need in the very competitive environment. The customized solutions offered by one of the best health care service provider in Bangalore - Futuristic Giga Tech Pvt Ltd range from patient access to collections help in improving the overall revenue cycle system of the clients. We assure to relieve much of your administrative and operational overhead and work towards increasing your profitability. With our years of experience being an offshore supporting vendor for our Healthcare clients at U.S. we analyze claims, every transaction and take all relevant actions to recover the amount due. We hold presence in the healthcare industry across payers, providers, healthcare services, e-health and government-funded programs which make it easy for us to handle the responsibilities and relieve you of the extra burden. Our value added Services include: RCM Service Billing Service Collection Service |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories
All
|



 RSS Feed
RSS Feed
